Single photon absorptiometry imaging as a screening method for diminished dual photon density measures

W.B. Cutler 1, J. Karp2 and R. Stine3
Maturitas, 10 (1988) 143-155
Elsevier Scientific Publishers Ireland Ltd.
Copyright ©1988 Elsevier Scientific Publishers Ireland
1. Athena Institute for Women's Wellness Research, Haverford, PA,
2. Hospital of the University of Pennsylvania, PA and 3. The Wharton School of the University of Pennsylvania, U.S.A
(Received 12 August 1987; revision received 20 October 1987; accepted 23 March 1988)
Scanning of the new 5-mm distal-radius site and the mid-radius (33% site) was performed using single photon absorptiometry (SPA) and of the L2-L4 region of the spine using dual photon absorptiometry (DPA) in a group of healthy women (ager range 36-66 yr ) in order to develop parameters to enable SPA to be used to screen for low DPA measures.
The study data were analyzed as follows:
1. Women were classified as either 'intact' or 'post pelvic surgery' and the data for the two groups were separated
2. Each SPA measurement was scrutinized and the one which produced the lowest score (% young normal YN) was entered for data analysis and graphing.
The application of these two analytical discriminators represents a new approach in the biomedical literature.
The findings were as follows:
1. When women were separated according to whether they were intact or had undergone pelvic surgery, the threshold value for screening using radius measures among intact women was set at 80% YN.
2. The necessary threshold value for the pelvic-surgery group needed to be set higher, at 93% YN.
3. If either the distal density or the mid-shaft density was below its threshold level, DPA was indicated.
4. At these threshold levels, no women with diminished spinal density (<83% YN) were omitted from screening procedure.
We conclude that by refining our evaluation of each healthy woman according to her pelvic physiology status (intact or post-surgery) and considering whether either of the two SPA measures is below the threshold value, we will be able to screen for diminished DPA density and thereby eliminate a significant number of expensive but uninformative DPA readings.
(Key Words: Single/dual photon absorptiometry, Screening, Density measures)
INTRO
Single photon densitometry (SPA) of the radius has not, so far, been proved useful as a tool for detecting deficient spinal density in women. However, because the procedures is less expensive, faster and physically more comfortable for the patient its use as a screening method would be welcomed by the medical community if it could be developed as an accurate tool in particular circumstances.
Although SPA has been shown to be capable of identifying bone loss in cross-sectional studies of several endocrine-related diseases [1-4], its use has been limited. Studies using quantitative computed tomography (QCT) evaluated the distal radial trabecular bone in osteoporotic and normal post-menopausal and normal pre-menopausal women [5]. The investigators concluded that the trabecular bone of the radius was equally as good a discriminator as the fibular trabecular weight-bearing region in revealing bone loss [5].
Cann [6] and Genant [7] evaluated 'mean peripheral mineral cumulative change' using SPA and reported that low doses (<0.625 mg) of conjugated equine estrogens revealed no response in the periphery within 2 yr following oophorectomy, whereas spinal measurements did so. Their peripheral measure was a combined average of the mid-radial and the 9/10 distal site. Thus, this study, which combined a predominantly cortical and partially trabecular site in evaluating response to very low estrogen doses, did not address the possible beneficial effect of usual estrogen replacement therapy does on individual predominantly trabecular SPA sites.
However, Christiansen et al. were able to: (a) demonstrate a positive SPA response to estrogen replacement therapy vs. placebo in an elegant crossover design among post-menopausal women who were followed up prospectively for 2 yr [8]; and (b) to demonstrate its efficacy in detecting change over time via repeated serial measures. [9].
Seven recent studies on the relationship between SPA (mid-radial and 9/10ths site) and dual photon absorptiometry (DPA) have been published [10-16]. All have revealed relationships between the two. None support the use of SPA as a sensitive screening method for changes in spinal bone mineral.
Recently, Grubb et al. [15] and Awbrey et al. [16] have developed applications for SPA at the 5 mm site. This is the locust at which the distal radius and ulna are separated by a distance of 5 mm. The use of rectilinear scanning permits efficient measurement of density at this site, although the site can still be located with more basic equipment. In their study of three groups of women with metabolic bone disease, Awbrey et al. suggested an at-risk level of 0.325g/cm for the 5 mm site to discriminate spinal osteoporosis. Perhaps most revealing was the accuracy advantage. Measurements at the new 5 mm site had only a 2% variation in each of the dimensions of mineral content width, and density, in contrast to significantly higher variations at the 9/10 site (7%,12%, and 5%) or mid-radius (2%, 2.5%, and 4%) [16]. Because the new 5mm site might provide more useful information than the previously studied 9/10 site or mid-radius, the 5 mm site was used in this study.
To date, all studies that have attempted compare SPA and DPA have sought to establish whether any one radial density site (9/10ths, 5 mm mid-radius, ultradistal) would provide a useful value for predicting DPA values. However, it has been repeatedly shown that bone loss does not follow a smooth progression at each site. One region may lose bone while another maintains it [5]. Accordingly, since each woman routinely provides two separate SPA values (5 mm site and mid-radius) it seemed appropriate to select the site which best revealed bone loss and to use it to compare this most revealing SPA measure with the one available DPA measure. By standardizing to 'percentage young normal' (% YN) for all values, previously undisclosed relationships might be revealed.
The investigators in the literature have made no systematic attempt to present data on the status of the women 's pelvic reproductive organs to indicate whether they were intact, hysterectomized, ovariectomized or had undergone tubal ligation. Although a few of the studies did evaluate post-oophorectomy patients, none compared whether the different populations were actually different from each other with regard to these bone density SPA/DPA relationships. In fact, only one of the seven studies which evaluated SPA vs. DPA made any mention of pelvic status [11] and in that investigation all the women were intact.
Pelvic status (intact vs. post-surgery) may well be a relevant variable in bone metabolism because of its relationship to the endocrine milieu. The incidence of pelvic surgery in the United States is four times higher than in six European countries [17, 18]. It is noteworthy that between 30% and 60% of menopausal patient populations will already have had pelvic surgery [19].
It has been known for some time that cardiovascular disease risk is significantly increased among women who have undergone hysterectomy with or without simultaneous bilateral oophorectomy [20]. A variety of post-hysterectomy defects, suggestive of endocrine alterations, have been reported, including increased incidence of depression, decreased beta-endorphin levels, loss of libido that does not respond to estrogen replacement therapy but may be responsive to testosterone, a rapid acceleration of aging of the skin and, at least in the case of oophorectomy, an accelerated rate of bone loss during the first 3 yr after surgery (for review see [19 and 21]). More recently, in 1987, it was shown that hysterectomy, with retention of the ovaries, produces an earlier menopause - on average 5 yr earlier than in age-matched intact control subjects [22]. The mechanism of ovarian failure is currently unresolved, although a developing literature provides data to suggest that the loss of neuroendocrine connections may contribute to the change in ovarian status (see [19] for review). Tubal ligation has also recently been shown to cause deficient estrogen levels.
Because pelvic surgery may alter the endocrine milieu in a woman and because the new 5 mm site has added to our ability to evaluate distal trabecular bone density, this report considers whether SPA might be developed in a useful way to serve as a method of screening for reduced DPA measures. Although Riggs et al. and Wahner et al. have demonstrated that the SPA 9/10ths and mid-radial sites are not deficient (> 2 S.D. below normal) among osteoporotic women [13, 24, 25] the question of whether a clinic population of healthy women might be usefully tested for diminished bone before the onset of advanced osteoporosis remains unanswered.
METHODS
The Women's Wellness Program at the Hospital of the University of Pennsylvania was started in March, 1986. Its purpose was to serve the medical needs of healthy women. The first 41 patients who passed through the center were offered dual photon densitometry as a service if they were having single photon densitometry. It was explained to each patient that the purpose of the dual photon study was twofold:
1. they would be supplied with information about their spinal density free of charge; and
2. the information would be useful in determining how well single photon densitometry reflected dual photon densitometry of the spine.
All patients were ostensibly healthy and had complete physical examinations with routine care as provided in the hospital program. Their age distribution (from 36 to 68) is shown in Fig. 1, which also displays the bone density range.
SPA and DPA were performed in all patients. Both the SPA and the DPA instruments used are manufactured by Lunar Radiation Corporation. The SPA unit uses and I-125 (28 keV) source, while the DPA unit uses an Gd-13 (44, 100 keV) source.
The SPA scans were performed at two sites, viz the mid-shaft site, which is one-third the distance from the ulnar styloid to the olecranon, and the 5mm site, which is the point at which the radius and ulna are separated by 5 mm. The percentage of trabecular bone relative to cortical bone is much higher at distal sites, such as the 5 mm site. The radius and ulna are scanned simultaneously, but we report results only for the radius. For the mid-shaft scan, 1.2 cm of bone length is averaged, corresponding to four scan lines of 0.3 cm length each. For the 5 mm scan, ten scan lines are recorded to be sure of including the line with 5 mm separation, but only this line is used in the analysis. The results are expressed as g/cm2 , which is often represented as BMC/W, or bone mineral content divided by the width of the bone, since the length and width of the bone scanned determines the area used to normalize the bone mineral mass. The BMC/W is then divided by the normal values for young women and expressed as the % YN.
The DPA scans extend from the iliac crest through vertebra L1, corresponding to 40 scan lines of 0.45 cm length each. The bone mineral mass is divided by the area scanned to give the area density, or bone mineral density (BMD). This value is generally reported for L1-L4, as long as none of the vertebral bodies has a compression fracture. Again, the BMD is divided by the normal value for young women and expressed as the % YN.
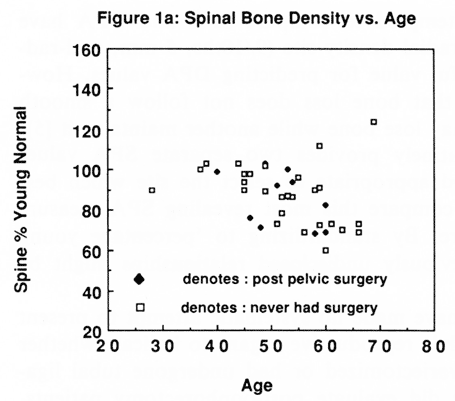
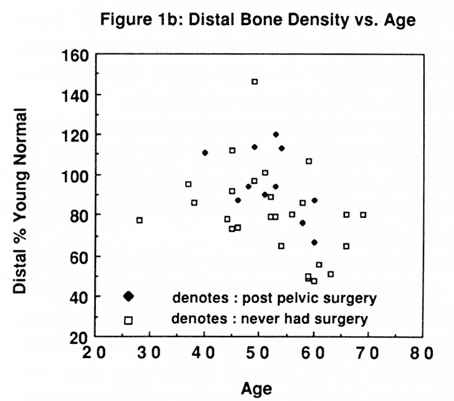
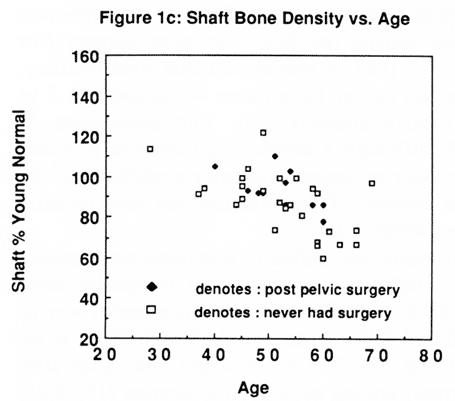
Fig. 1 (a-c). Density data for each patient by age for the spine, the distal 5 mm site and the shaft (% YN = percentage young normal). Spine % YN (intact patient); Spine % YN (pelvic surgery patient).
The reproducibility (also called 'precision') of these techniques has been measured at the Hospital of the University of Pennsylvania by the Department of Nuclear Medicine. The percentage coefficient of variation (% CV) was found to be 1-2% for SPA and DPA, which includes uncertainties in patient repositioning and data analysis. This is consistent with results reported elsewhere [24]. It may be more relevant, however, in comparing two measurements at different sites, to consider the accuracy of the techniques. The accuracy, which is determined by comparing the absorptiometric measurement of the BMD with an absolute measurement, such as ashed weight determinations of density, is about 3% for DPA and 6% for SPA [26,27].
The study data were analyzed as follows:
1. women were classified as either 'intact' or 'post pelvic surgery' and the data for the two groups were separated; and
2. each SPA measurement was scrutinized and the one which produced the lowest score (% YN) was entered for data analysis and graphing.
The application of these two analytical discriminators represents a new approach in the biomedical literature. We believe these two discriminants to be critically important in providing a means of establishing the use of SPA as an economically valuable screening method for diminished DPA spinal density measures.
RESULTS:
Table 1 provides the data on the patients investigated. Figures 1a-c show density data by age for each patient for the spine, the distal 5 mm site and the shaft respectively. Different symbols are used to indicate the intact and the post surgery patients.
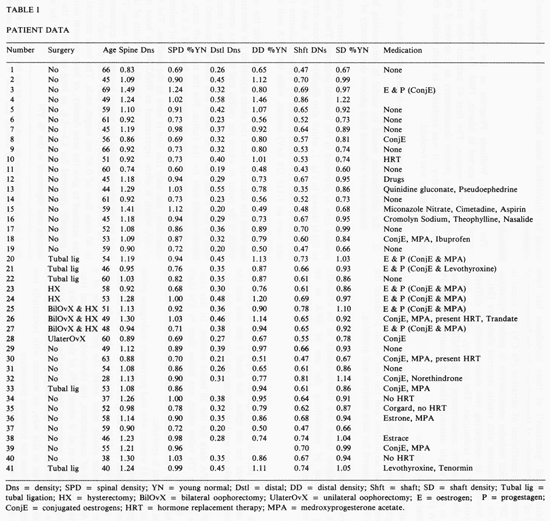
Figure 2 shows the DPA vs. SPA data for the 30 intact women. In this sample, 21 women showed a distal % YN value which was below their % YN shaft value. It is noteworthy, however, that 9 women showed a % YN shaft value, which was lower than their distal value. Such data are in accordance with the previous observations that bone loss is sporadic.
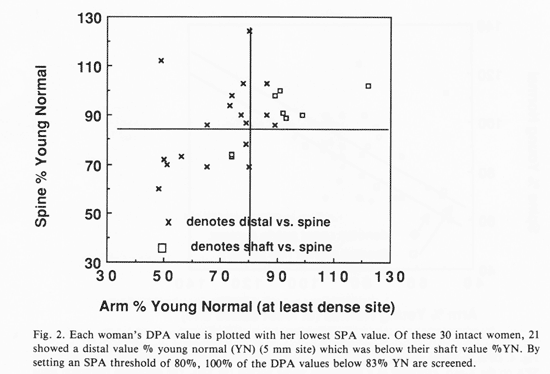
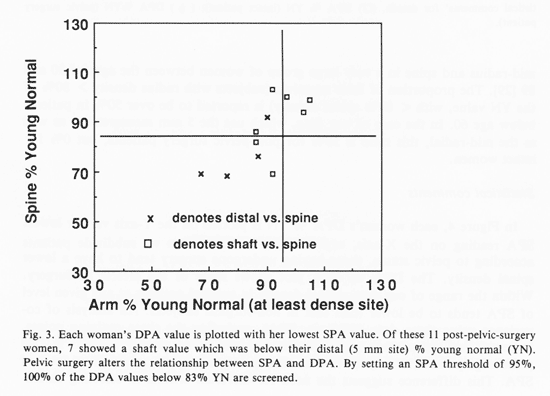
Figure 3 shows the data for the 11 women who had previously undergone pelvic surgery. When we distinguish between the women according to pelvic status, two separate thresholds can be established for revealing DPA %83 or less on the basis of these data. Although we have taken 83% as a threshold value, it is an arbitrary figure and a more appropriate choice must await the performance of a larger series of studies. As a basis of comparison, the threshold for spinal fracture of 0.97 g/cm2 reported by Melton et al. is about 78% of the YN density. We note that the SPA threshold for intact women in these data lies at about 80% of the YN value, while the SPA threshold for post-surgery women is higher, at 93%. When threshold values are set in this way, no women with potentially low spinal density would be excluded from the screening procedure.
It is worth comparing our data with those of Ettinger et al., who measured the mid-radius and spine in a very large group of women between the ages of 30 and 89 [29]. The proportion of false negatives (subjects with radius density > 80% of the YN value, with < 80% spinal density) is reported to be over 50% in patients below age 60. In the case of our data, which use the 5 mm measurement as well as the mid-radial, this ratio is 50% for post-pelvic surgery patients, but 0% for intact women.
Statistical comments
In Figure 4, each woman's DAP % YN is plotted on the Y-axis vs. her lowest SPA reading on the X-axis, expressed as %YN. When we subdivide patients according to pelvic status, those having undergone surgery tend to have a lower spinal density. The DPA vs. SPA plot shows some of the effects of surgery.
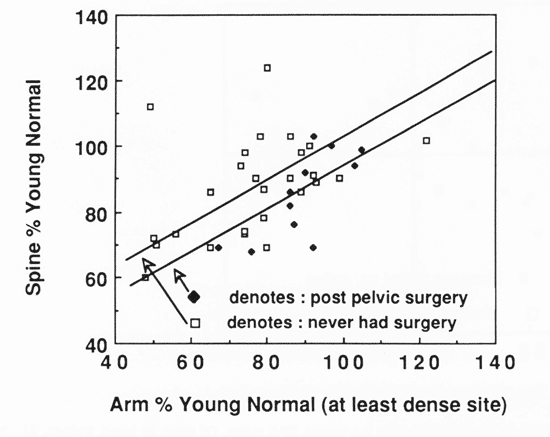
Within the range of our data, spinal density in surgical patients at any given level of SPA tends to be lower than that in non-surgical subjects. An analysis of covariance using these data (DPA vs. SPA), excluding the three outlying points, indicates that the average spinal density for post-pelvic surgery subjects is 7.00 percentage points (+ 3.6) lower than that in intact subjects at any given level of SPA. This difference suggests the need for different criteria in selecting thresholds to identify patients with low spine density. Since the surgical group tend to have lower spinal density than the non-surgical group at any given level of SPA, we have to use a higher threshold point for the surgical than the non-surgical patients in order to reduce the false positive rate of classification.
The analysis of covariance findings suggests shifting the threshold by 12.1 + 6. This estimate derives from the ratio 7 divided by 0.58 + 0.1 is the regression slope of DPA on SPA and the 7 reflects the average 7 percentage points difference referred to above. This 12.1 + 6 estimate is thus very close to the 13 percentage points threshold difference indicated in the results section.
We note that there is some indication that the slope is steeper in surgical than in non-surgical patients, but the effect is not significant because of the small sample size. The slopes are therefore treated as equivalent and thus provide parallel regression lines in the two groups.
CONCLUSION
The data for each woman were considered in three dimensions:
1. distal SPA density, percentage young normal (% YN);
2. mid-radial SPA density (% YN); and
3. pelvic status (hysterectomy, ovariectomy, tubal ligation, or intact)
The results showed the following:
1. When women were separated according to whether they were intact or had undergone pelvic surgery, the threshold value for screening using radius measures among intact women could be set at 80% YN.
2. The necessary threshold value for pelvic-surgery subjects needed to be set higher, at 93% YN.
3. If either the distal density or the mid-shaft density was below its threshold level, DPA was indicated.
4. At these threshold levels, no women with diminished spinal density (<80% YN) were omitted from the screening procedure.
Future studies should serve to refine the appropriate threshold SPA measures so as to eliminate false negatives and minimize wasteful tests.
We hope that other investigators will consider evaluating their data according to the two new parameters presented here. By considering a patient's pelvic status and then evaluating whether she is below the threshold for either of the two SPA measures, we hope to achieve a better understanding of the relationship between bone loss in the spine and arm and possibly be able to carry out efficient screening of a certain subclass of patients for diminished dual photon densitometry.
Judging from a visual scan of our own data (see Figs.2 and 3), we would conclude that if others replicate the general pattern presented here, we might expect it to be possible to dispense with the need for spinal readings in a significant number of women between the ages of 45 and 60 as a result of single photon densitometry screening.
Since it is precisely during this period of life that rapid acceleration of spinal bone loss most frequently occurs, a valuable economic role for SPA as a screening method may in fact be established in this age group. In the case of women over the age of 60, more data are desirable. SPA may become useful for women in the over 60-population who begin using hormone replacement therapy. In this group, it would probably be very useful to know whether bone diminution halted. These preliminary data are presented in the hope that others will follow the lead offered and provide either a confirmation or a demonstration that the method described can be improved.
ACKNOWLEDGEMENTS
We thank Abass Alvi, M.D., Chief of Nuclear Medicine and Frederick Kaplan, M.D., Chief of Metabolic Bone Disease at the Hospital of the University of Pennsylvania for their encouragement, comments, and cogent criticisms of earlier drafts of this manuscript.
References
1. Adinoff, A, Hollister JR. Steroid-induced fractures and bone loss in patients with asthma. New Engl J Med 1983; 309: 365-368
2. Aloia, JF, Vaswani AN, Yeh JK, Ross P, Ellis K, Cohn SH,. Determinants of bone mass in postmenopausal women. Arch Intern Med 1983;143:1700-1704.
3. Meema S, Meema HE. Evaluation of cortical bone mass, thickness and density by z-scores in osteopenic conditions and in relation to menopause and estrogen treatment. Skeletal Radiol 1982; 8: 259-268
4. Hahn, TJ, Boisseau VC, Avioli LV. Effect of chronic corticosteroid administration on diaphyseal and metaphsyseal bone mass. J Clin Endocrinol Metab 1974; 39: 274-282
5. Reugsegger P, Dambacher MA, Reugsegger E, Fisher JA., Anliker M. Bone loss in premenopausal and postmenopausal women. J Bone Jt Surg 1984; Inc. 66-A:7: 1015-1023
6. Cann CE, Genant HK, Ettinger B, Gordan GS. Spinal mineral loss by quantitative computed tomography in oophorectomized women. J Am Med Assoc 1980; 244: 2056-2059
7. Genant HK, Cann CE, Ettinger B, Gordan GS. Quantitative computed tomography of vertebral spongiosa: A sensitive method for detecting early bone loss after oophorectomy. Ann Intern Med 1982; 97: 699-705
8. Christiansen C, Christensen MS. Bone mass in postmenopausal women after withdrawal of estrogen/gestagen replacement therapy. Lancet 1981; I: 459-461.
9. Christiansen C, Riss BJ, Rodbro P. Prediction of rapid bone loss in postmenopausal women. Lancet 1987; I: 1106-1110.
10. Seeman E, Wahner HW, Offord KP, Kumar R, Johnson WJ, Riggs BL. Differential effects of endocrine dysfunction on the axial and the appendicular skeleton. J Clin Invest 1982; 69: 302-1309.
11. Nilas L, Borg J, Gotfredsen A, Christiansen C. Comparison of single and dual photon asborptiometry in postemonpausal bone mineral loss. J Nucl Med 1985; 26:1257-1262.
12. Madsen M. Vertebral and peripheral bone mineral content by photon absorptiometry. Invest Radiol 1977; 12:185-188.
13. Riggs BL, Wahner HW, Dunn WL, Mazess RB, Offord KP, Melton LJ. Differential changes in bone mineral density of the appendicular and axial skeleton with aging. J Clin Invest: 1981; 67: 328-335.
14. Krolner B, Nielsen SP, Lund B, Lund BJ, Sorensen OH, Uhrenholdt A. Measurememnt of bone mineral content (BMC) of the lumbar spine. Correlation between forearm BMC and lumbar spine BMC. Scan J Clin Lab Invest 1980; 40: 665-670.
15. Grubb SA, Jacobson PC, Awbrey, BJ, McCartney WH, Vincent IM, Talmage RV. Bone density in osteopenic women: A modified distal radius density measurement procedure to develop an " at risk" value for use in screening women. J Orthopaed Res 1984; 2: 322-327.
16. Awbrey BJ, Jacobson PC, Grubb SA, McCartney WH, Vincent IM, Talmage RV. Bone density in women: a modified procedure for measurement of distal radial density. J Orthopaed Res 1984; 2: 314-321.
17. Fortney J. Fam Plann. Perspect. 1987; 19:1.
18. van Keep PA, Wildemeersch D, Lehert P. Hysterectomy in six European countries. Maturitas 1983; 5: 69-75.
19. Cutler WB, Garcia CR. Perimenopausal bleeding and hysterectomy. In: The medical management of menopause and premenopause: their endocrinologic basis, Chapter 8. Philadelphia: Lippincott, 1984.
20. Cutler WB, Garcia CR. Hormone replacment therapy and coronary heart disease. In: the medical management of menopause and premenopause: their endocrinologic basis, Chapter 6. Philadelphia: Lippincott, 1984.
21. Cutler WB, Hysterectomy: Before and After. New York: Harper and Row, 1988.
22. Siddle N, Sarrel P, Whitehead M. The Effect of hysterectomy on the age at ovarian failure: identification of a subgroup with premature loss of ovarian function and literature review. Fertil Steril 1987; 42: 94-100.
23. Cattanach J. Estrogen deficiency after tubal ligation. Lancet.: 1985; I: 847-849
24. Riggs BL, Differential effects of endocrine dysfuncton on the axial and the appendicular skeleton. J Clin Invest 1982; 69: 1302-1309
25. Wahner HW, Dunn WL, Riggs Bl. Assessment of bone mineral. Part 2. J Nucl Med 1984; 25: 1241-1253.
26. Wilson CR, Madsen M. Dichromatic absorptiometry of vertebral bone mineral content. Invest Radiol 1977; 12: 180-184
27. Cameron JR, Mazess RB, Sorenson JA. Precision and accuracy og bone mineral determination by direct photon absorptiometry. Invest Radiol 1968; 3: 141-150
28. Melton LJ, Wahner HW, Richelson LS, O'Fallon WM, Dunn WLL, Riggs BL. Bone density specific fracture risk: A population based study of the relationship between osteoporosis and vertebral fracures. J Nucl Med 1985; 26: 24.
29. Ettinger M, Mazess RB, Barden HS. Insenstivity of peripheral measurement to spinal osteopenia. Presented at the AM. Soc. Bone Min Res. CA: Anaheim, June 1986.