Conclusions
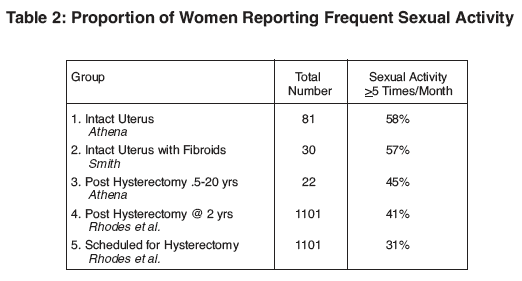
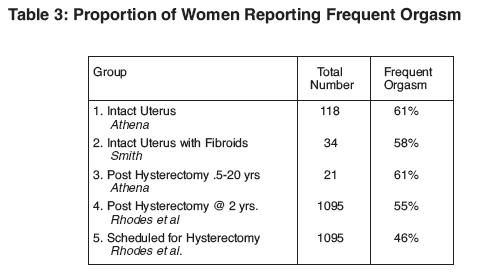
1) Sexual life is apparently suppressed in women scheduled for hysterectomy. Our data show that not only are women less likely to engage in frequent sexual activity before hysterectomy, but when they do have sexual relations they are less likely to experience orgasm.
2) In women who consent to hysterectomy, a combination of unstudied factors (e.g. pain, bleeding, fear of surgery) apparently combine to reduce their sexual activity.
3) The current practice1,2 of comparing immediate pre-surgery baselines of reduced sexual activity with data collected 1 to 2 year post surgery gives rise to an inherently erroneous conclusion.
4) Future outcome studies after hysterectomy must correct the design errors of previous research. While a woman's prior healthy sexual life history would provide an ideal baseline, such data from distant recall have questionable validity. Hence a valid presurgical baseline is practically impossible to obtain.
5) Future studies of sexual life should compare women after healing from hysterectomy to groups of women with comparable conditions who have not undergone reproductive surgery. Because both groups could provide prospective current information of relatively healthy patterns of sexual behavior, such measures could explore further the effect of hysterectomy on sexual life of women.
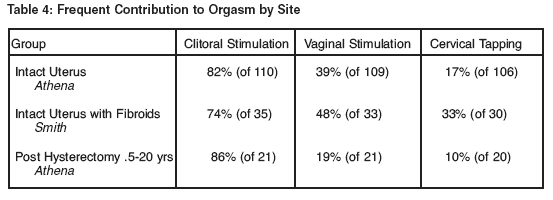
6) Hysterectomy does not seem to impair clitoral sensation but does result in reports of reduced vaginal and cervical sensation
7) Women undergoing hysterectomy because of myomata uteri, should be told that the surgery may reduce their genital sensitivity since this condition is associated with enhanced genital sensitivity
References
1. Rhodes JC, Kjerulff KH, Langenberg PW, Guzinski GM (1999) Hysterectomy and sexual functioning. JAMA 282:1934-1941
2. Carlson KJ, Miller BA, Fowler FJ (1994) The Maine Women'sHealth Study: I. Outcomes of hysterectomy. Obstet Gynecol 83:556-65.
3. Master WH and Johnson VE (1966) Human Sexual Response Little, Brown, Boston
4. Alzate H (1985) Vaginal eroticism: a replication study. ArchSexBehav 14:529-537. and for example,
Alzate H (1985) Vaginal eroticism and female orgasm: a current appraisal. Journal of Sex and Marital Therapy 11:271-284.
5. Komisaruk B, Whipple B (1986) Vaginal stimulation - produced analgesia in rats and women. Annals NY Acad. Sciences 467:30-39. and
Komisaruk BR, Gerdes C, Whipple B (1997) Complete spinal cord injury does not block perceptual responses to genital self stimulation in women. Archives of Neurology 54:1513-1520.
6. Cutler WB, McCoy NL, Friedmann E, Genovese-Stone E, Zacher MJ (2000) Sexual response in women. ObstetGyncol 95:4(Supplement) April 2000, 198.
7. Cutler WB, Friedmann E, Genovese-Stone E, and Felmet K (1992) Urinary stress incontinence: a pervasive problem among well women. J Wmns Health Vol 1:259-266.
8. McCoy NL and Matyas JR (1996) Oral contraceptives and sexuality in university women. ArchSexBehav 25:73-90.
9. PROZAC (fluoxetine HCL) prescribing information by Dista/Eli Lilly, pp. 859-863, PHYSICIANS DESK REFERENCE 52nd Ed (1998), Medical Economics Company, Inc. Montvale, NJ 07645.
RELATED INFORMATION ON ACOG: Visit www.acog.org