Prevalence of Kyphosis in a Healthy Sample of Pre and Postmenopausal women

Winnifred B. Cutler PhD.
Erika Friedmann, Ph.D. and Elizabeth Genovese-Stone, MD
American Journal of Physical Medicine & Rehabilitation
Copyright ©1993 by Williams & Wilkins
ABSTRACT Cutler, WB, Friedmann E, Genovese-Stone E, Prevalence of kyphosis in a healthy sample of pre- and postmenopausal women. Am J Phys Med Rehabil 1993; 72:219-225
Kyphosis, initially modest, progresses to the well-recognized dowager's hump of the postmenopausal osteoporotic woman. Kyphosis is not only associated with relatively altered vertebral body shape (anterior wedging), but also with reduced bone density and fitness, as well as decreased muscle strength, and is associated with reduced survival. We found an unexpectedly high (35%) incidence of kyphosis in a healthy sample of well women 20 to 64 years of age. The correlation between normal postural index of kyphosis (I/K) and upright postural I/K was substantial (r=0.799). Among the postmenopausal women, normal postural I/K was inversely correlated with age. Upright postural kyphosis was not related to age, nor was normal postural I/K in the premenopausal woman.
There was no direct relationship demonstrated between current calcium consumption and I/K. Similarly, neither estrogen levels nor follicle-stimulating hormone levels were related to current posture. Women with satisfactory exercise habits had significantly lower I/K.
Because the capacity to stand up straight was consistently higher than the normal postural score, yet closely correlated to it, there may be a role for postural kyphosis in changing the architecture of the vertebral columns. As normal posture becomes kyphotic, an individual can no longer straighten the vertebral column.
The surveyor's flexicurve, which we employed for this study, provided a simple and inexpensive method for assessing postural index. This measurement can be routinely included in the comprehensive health examination. Assessment of bone health in women should be made within the context of a fixed postural kyphosis.
KEY WORDS: Menopause, Kyphosis, Flexicurve, Osteoporosis
Intro:
Studies of the architecture of the vertebral column have revealed associations with osteoporosis in post-menopausal women and men after the age of 49 years. Morbidity with significant back pain and limited mobility is common in older men and women.1-5 By the age of 55 years, 29% of women acknowledge significant back pain in large sample studies. 6 Back pain is associated with loss of height; 50% of adults who have lost height report pain. 6
Kyphosis, initially modest, progresses to the well-recognized dowager's hump of the postmenopausal osteoporotic woman. The mechanism of kyphosis is presumed to occur through anterior thoracic compression fractures and the subsequent formation of a compensatory fat pad. Kyphosis is not only associated with relatively altered vertebral body shape (anterior wedging), but also with reduced bone density and fitness, as well as decreased muscle strength, and is associated with reduced survival 7-12.
There is a paucity of literature evaluating early postural kyphosis in the bone health of premenopausal women. In fact we found no studies in the literature reporting the incidence of kyphosis in women before the age of 49 years. Because research is now focusing on the potential of prevention of these progressive bone debilities, a study of the normal timing of the development of kyphosis seemed particularly timely. We wished to study the timing of the development of kyphosis in normal women. We have examined the incidence of kyphosis to pose the following questions: (1) What is the incidence of kyphosis in a well women population? (2) Is the degree of kyphosis and age related among pre- or postmenopausal women? (3) Is normal posture index of kyphosis (I/K) correlated to upright postural I/K? (4) Is I/K related to hormone levels (follicle-stimulating hormone or estrogen), to current dietary calcium or exercise habits?
METHODS
The Population
We studied the data from 140 consecutive female subjects at the Athena Wellness Program (a comprehensive physical examination that also reviews behavioral habits and subject history). The subjects ranged in age from 20 to 64 yr and were presumably in good health. Postural data was provided by 136 subjects.
These healthy women were participating in an 'executive level' comprehensive physical examination; an annual physical examination for well women. Because the price for this 2.5 h wellness evaluation exceeds $300.00, the population is either composed of corporation-paid management-executive level women or those choosing the examination independently. Thus, the women tended to be of high socioeconomic status.
Overview of Procedures
Each woman was asked to complete preprinted forms, as well as consent to an interview and examination. Medical history forms completed by the subject and physical file notes were subsequently reviewed and coded to extract data concerning age, physician recommendations for exercise, dietary habits and laboratory test results. The index of kyphosis (I/K) for both normal and upright posture was measured by a trained technician. For kyphosis assessment with the flexometer we asked the subject to stand the way she normally does (normal posture); then to stand as straight as possible (upright posture).
Measurement of Index of Kyphosis using the Flexometer
We followed the methods of Chow and Harrison7 and Milne and Lauder 10 and Milne and Williamson.11 Index of kyphosis was designed to provide a score that indicates the degree of curvature of the upper spine. A score of 7 or less is associated with erect posture. A score of 10 or higher reflects curvature; with the higher numbers, 11 or more, indicating increasingly greater deformity. Briefly, a 60 in plastic-covered surveyor's flexicurve “the flexometer' (which bends in one plane and holds its shape) was laid against the C7 protuberance and shaped along the spine to the thoracicolumbar joint. Once molded to the spinal posture of the subject, the flexicurve was lifted and laid on a ruled sheet of paper such that the cephalic end (C7 position) was placed at the left on the line and the thoracicolumbar joint position was placed at the right on the same line. By doing this, two curves cross the line. The flexicurve was then outlined in pencil on the paper and an index of kyphosis was calculated by measuring the largest height and dividing by the largest width of the line intersected from the thoracic region of the back. This number is multiplied by 100 to yield an integer score (see Fig. 1). The index of kyphosis has been previously shown to be highly reproducible and reflective of bone mass in the spine in postmenopausal women and elderly men. 7, 10, 11
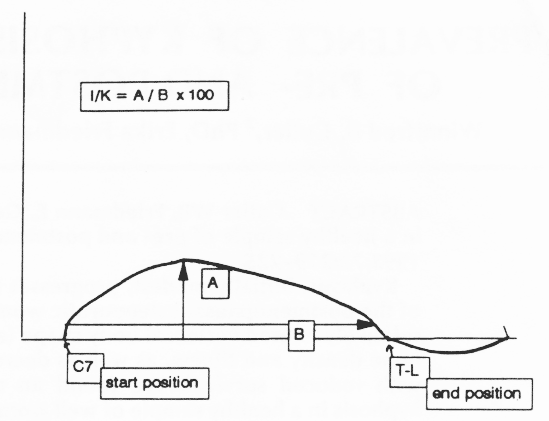
Figure 1. The measurement of index of kyphosis. The flexicurve is first laid against the C7 protuberance and shaped along the spine to the thoracicolumbar joint. Once molded it's laid on a ruled sheet of paper such that the cephalic end is placed at the left on the line (at the first “X”) and the thoracicolumbar joint position is placed at the right on the same line (wherever it crosses the line becomes the second “X”). This curve is outlined in pencil on the paper. The I/K calculation equals the largest height (A) divided by the width (B) multiplied by 100 to yield an integer score.
Two tracings of this flexometer are performed; one for the normal relaxed posture and one for the best upright posture the subject can hold. Incidence of normal postural kyphosis was determined according to I/K thresholds previously described. 7,10, 11
Medical History Questionnaire Completed by Subject
History is obtained by questionnaire and by interview. Initially the subject is mailed a “subject medical record” form that she is asked to complete. The form asks questions regarding name, address, occupation history, education, marital status, chief complaints and family history. It provides sufficient spaces labeled for first degree relatives and spouse(s) current age and health as well as age at death and its cause. A list of the 10 most common, potentially heritable diseases is provided with space to answer if and which blood relative have had them. The medical record form then provides a self-scoring checklist of 30 diseases, a range of potential allergies, injuries and transfusions; these are to be checked “yes” or “no”. Similarly a section on past surgeries gathers surgical history and a section on "systems" gathers history of problems with eyes, ears, respiratory, glandular, psychogenic, cardiovascular, incontinence, pains, digestive and other psychophysiologic systems. Next there is a section to assess habits including sleep, exercise pattern, smoking, drinking and drug use. Sections on gynecologic history, obstetric history, sexual history and contraceptive history precede a 'personal history' section; as well as a history of psychotherapy. Time since (and reason for) entry into menopause (e.g., surgery) is available from several different questions; these include gynecologic history and surgical history. A hormonal lability test allows the subject to self-score the Kupperman Menopausal Index, a validated test for hot flashes and other perimenopausal symptoms that has been closely correlated to estrogen levels of pre- and postmenopause. 12 The medical history form concludes with a calcium/vitamin D questionnaire (The Athena Calcium Questionnaire) shown in Table 1. The form requires about 45 min to complete. The form states clearly that all data will be coded anonymously for subsequent study, data analysis, and potentially be used to contribute to biomedical knowledge. Subject confidentiality is maintained.
TABLE 1
Athena Calcium Questionnaire
| Circle the response and the number following each response which best answers each question. Place the number in the blank to the right of each question and add up your score at the end of the questionnaire. | ||
1. |
How many (8 ounce) servings of milk (regular, skim, low-fat) do you drink daily? Less than one (0) One (3) Two (6) Three (9) Four or more (12) | |
2. |
How many servings of cheese do you have daily? (one serving = 1 ounce, 1 slice, 1-inch cube). Do not include cottage, ricotta, or cream cheese here. Less than one (0) One (3) Two (6) Three (9) Four or more (12) | |
3. |
How many servings of yogurt, pudding, or custard (one serving = 1 cup) or ricotta cheese (one serving = 1/2cup) do you have each week? Less than one (0) One (0.5) Two (1) Three (1.5) Four or more (2) | |
4. |
How many servings of cottage cheese do you have each week? (one serving - 1/2 cup)Less than one (0) One (0.15) Two (0.3) Three (0.5) Four or more (1) | |
5. |
How many servings of canned sardinges or salmon (with bones) do you have each week? (one serving = 3 ounces).Less than one (0) One (0.5) Two (1) Three or more (1.5) | |
6. |
How many servings of the following vegetables do you have each week? ( one= 1/2 cup cooked). Greens: collards, kale, mustard, turnip, or beet; chard, excarole, spinache, boccoli, bean sprouts, okra, lettuce (dark green), cooked beans (kidney, pea lima chick pease), lentils. Less than one (0) One (0.2) Two (0.5) Three (1) Four (1.5) Fiver ormore (2) | |
7. |
How many servings of ice cream (hard or soft serve), ice milk, or frozen yogurt do you have each week? (one serving = 1/2 cup).Less than one (0) One (0.1) Two (0.3) Three (0.5) Four or more(1) | |
8. |
Do you take a calcium supplement regularly? Yes/No. If yes brand___, Amount per day_____ |
|
9. |
Do you take a multivitamin/mineral tablet regularly? Yes/No If yes, brand____ |
|
10 |
Do you spend 15 minutes or longer each day out of doors in the sunlight? Yes/No |
Dietary Calcium
A ten-part calcium questionnaire is completed by each subject (see Table 1). Scoring evaluates average calcium consumption per day. Scores are designed to produce a total score that reflects hundreds of milligrams of calcium ingested per day. For reference to calcium nutrition tables and calories see Ref. 12.
The Subject Interface with Clinical Staff
At the time of appointment, an intake counselor reviews the completed form and helps the subject complete any parts that were left blank. Later, when the subject is medically examined, additional comments are entered directly on the medical history form by the clinician to affirm or assess the doctor's reaction to the entries on the medical history form. These subject files are subsequently examined at the research institute. Data are coded onto a computerized database for subsequent graphing and analysis.
Hormones
When subjects requested hormone testing (e.g., estrogen, follicle-stimulating hormone, thyroid), or the physician judged it relevant, blood was drawn during the physical examination and sent to SmithKline Laboratories for assay. Radioimmunoassay results are sent both to the physician and the research institute for data entry intended for subsequent scientific review. For this report, all hormone data concerning the sex hormones (follicle-stimulating hormone FSH and estrogen) were extracted from the database records described above.
Data Retrieval
Student interns record all subject data onto computer databases using numerical codes (entered onto Framework III software). Framework later is exported to Lotus for subsequent analysis. The databases are then imported into a QuatroPro 4.0 environment for graphing. Similarly the databases are uploaded onto an IBM main frame for statistical testing using SPSS.
Statistical Assessment
X2 statistics were calculated to examine differences in frequencies for categorical variables. Pearson's correlation coefficients were used to examine the relationship between continuous variables. Regression analyses were utilized to derive slope and Y intercept where relevant. Student's t tests were utilized to examine differences in averages between groups.
RESULTS:
Kyphosis measurements of both upright and normal posture were available for 136 women. Figure 2 shows the age distribution of the study sample.
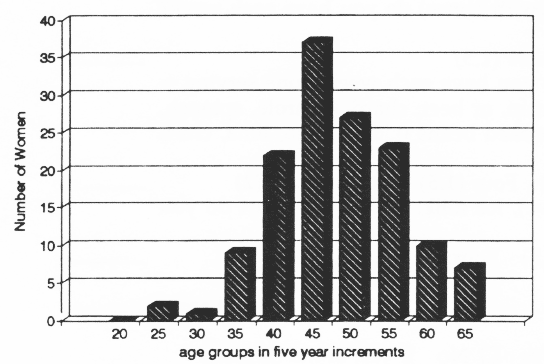
Figure 2. Age distribution of the sample shown in 5-year increments. The age on X axis represents the upper age limit of the 5-year span
Kyphotic Index: Normal Posture v Upright Posture
Figure 3 shows each woman's two flexometer scores (normal v upright I/K). Normal posture is closely and significantly correlated to upright posture r= 0.7955 (slope = 0.7982; Y intercept = 0.2471) P< 0.001, n=136.
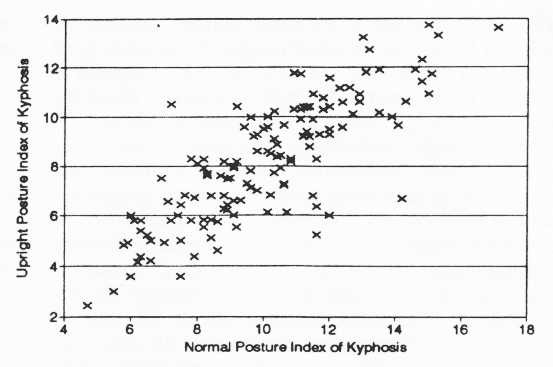
Figure 3. The relationship between normal and erect postural kyphosis. The entire sample of 136 women show a close relationship between their normal postural kyphosis and their capacity to stand upright.
The close correlation between normal and upright index of kyphosis is preserved when the groups are dichotomized according to menopausal status and evaluated separately (premenopausal women r= 0.8200, P = 0.0001, n=94; postmenopausal women r = 0.7720, P=0.0001, n=37)
Incidence of Kyphosis
A normal postural I/K >10, in a woman's normal stance is reasonably reflective of stooped back. According to that criterion, 51% of our sample is kyphotic. According to a more conservative threshold, an I/K > 11, 35% of this sample is kyphotic.
Relationship of Age and Menopausal Status to Kyphosis
Figure 4 shows the age distribution v the normal postural index of kyphosis in these 136 women. Age shows no continuous relationship to kyphosis in either normal posture or upright (r = -0.1427 for normal posture; r = - 0.0927 for upright posture).
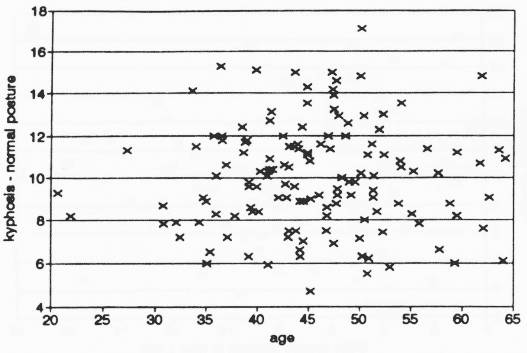
Figure 4. The distribution of normal 1/K by age. The entire sample of 136 women range from 20 to 64 years. No relationship between age and kyphosis is observed in this healthy sample of women.
However, when the population is dichotomized (pre - v postmenopausal), one significant correlational relationship occurs in the postmenopausal group. Among the 39 postmenopausal women, chronologic age (but not years since onset of menopause) does show a weak but significant relationship to normal posture (r = -0.3056, P = 0.025). Paradoxically those who are older tend to have better normal posture in this sample. The upright kyphotic index showed no such relationship (r = -0.0998).
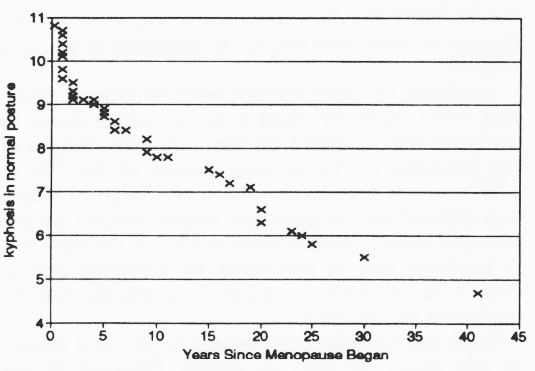
Figure 5. The distribution of normal 1/K by years in postmenopausal women. Menopausal age is not significantly related to degree of normal postural kyphosis in this sample.
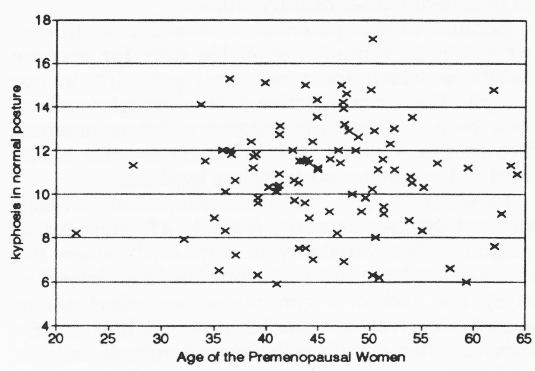
Figure 6. the distribution of normal 1/K by age among premenopausal women. This sample of 94 women who have not yet entered menopause show no significant relationship between age and normal postural kyphosis.
Figure 5 arrays the age distribution v kyphosis in the 39 postmenopausal women according to years since entry into menopause. Figure 6 arrays the similar data of 94 premenopausal women according to their chronologic age and normal postural index of kyphosis.
The group average index of kyphosis in normal posture is significantly higher in the postmenopause group than the premenopausal group {t(133) = 1.98, P =0.05}. The average normal-posture premenopausal kyphotic index for 94 women was 9.77 (0.244 SEM); the average postmenopausal kyphotic index for the 39 women was 10.67 (0.40 SEM). Upright posture I/K was not significantly different in the pre-v the postmenopausal group per t test. Thus the data show no simple correlation between increasing age/menopausal stage and kyphosis. In support of greater I/K in the menopausal women is a higher group mean I/K for normal posture in postmenopause compared with premenopause. Opposing this result is our finding that individual (correlational) data show a reverse trend in postmenopausal women. Older "well women” undergoing executive examinations show better posture than younger postmenopausal women.
Sex Hormones and Kyphotic Index
Hormone levels were not related to kyphotic index in this sample. Follicle-stimulating hormone level (n = 41) and estrogen level (n= 26) showed no significant correlations with normal or upright I/K. Estrogen level was negatively correlated with age (the entire sample: r = -0.3150, n = 26, P = 0.059; the postmenopausal group: r = -0.4955, n = 11, P = 0.059). It should be emphasized that women requesting hormone tests usually did so because of questions about possible menopausal status. Thus these are not random samples.
Dietary Calcium and Kyphotic Index
Estimated calcium consumption per day is plotted in Figure 7 along the X axis. Less than half this sample achieve minimum recommended levels of 650 mg/day. The calcium in the current diet was not related to either normal or erect kyphosis. The entire group showed no relationship between calcium and kyphosis for upright posture (r = -0.0463). For the normal postural index (r = -0.0742) see Figure 7a.
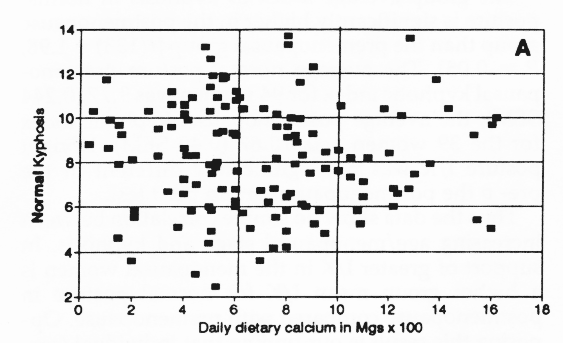
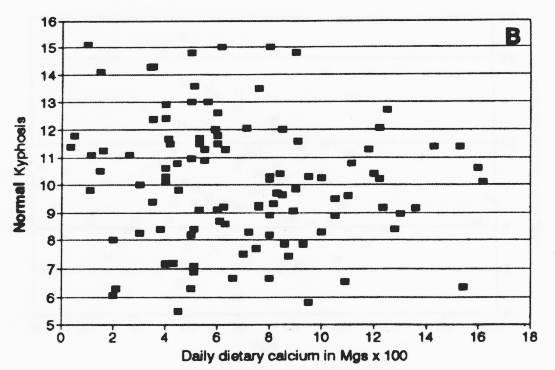
Figure 7. Dietary calcium intake v kyphosis (A) and dietary calcium intake for nonsupplement users (B). No obvious relationship was observed between current dietary calcium habit and postural scores.
Of the 137 subjects, 29 (21%) used calcium supplements of different brands and doses. Because calcium supplements are not uniformly soluble, 12 we generated a second graph of dietary calcium v I/K to observe whether nonsupplement users showed a different pattern from all the women.Nonsupplement users showed a similar nonrelationship to kyphosis as shown for the entire sample.
Dichotomizing the population revealed no other relationship between calcium and I/K: premenopausal women calcium (and normal posture r = -0.0630; upright r = -0.0174); postmenopausal women (normal posture r = -0.0862; upright posture r = 0.1187).
Exercise Prescription and Kyphotic Index
Analysis showed that the physician tended to prescribe more frequently for subjects whose normal I/K was >13 than for women with better posture (x2 (1, n=138) = 3.43, P <0.05 one-tailed). The physician's prescription to exercise did show a modest relationship to postural score. The physician prescribed exercise for those subjects identified as sedentary.
DISCUSSION
Our studies of postural kyphosis reveal an unexpectedly high index of kyphosis in a healthy population of women ranging from age 20 to 64 years. We find that between 35% and 51% of the population is kyphotic in their normal posture (depending on the threshold score we choose for defining kyphosis). A substantial correlation between normal postural index of kyphosis and erect postural index of kyphosis was demonstrated. In our well-women population, the more then habitual posture is shown to be kyphotic, the greater the likelihood that an individual cannot stand up straight. Because the capacity to stand up straight was consistently higher than the normal postural kyphotic index, there may be a role for bone remodeling in habitual postural kyphosis.
Kyphosis was not age dependent. It was common well before the menopause, when one in three women has significant kyphosis. Although the majority of this sample do not consume the recommended dietary allowances for calcium there was no direct relationship demonstrated between current calcium consumption and kyphosis. Our result is consistent with several other studies, which (at variance with the breadth of the literature (for review see Ref. 12)) have found no relationship between dietary calcium and indicators of bone mass 13-15. Similarly neither estrogen levels nor follicle-stimulating hormone levels revealed relationships to current posture in our population of women under age 65.
The literature has suggested a possible relationship between kyphosis and bone remodeling. After age 49 years, bone density is inversely related to kyphosis according to bone mass studies using total body calcium, 7 and dual photon absorptiometry of the L2-L4.16 No data have been published on the density of bone with respect to kyphosis in younger women.
Kyphosis has been studied with relation to vertebral body shape by chest x-ray in which index of wedging was analyzed by comparing the length of the posterior to the anterior border of the 7th to 12th thoracic bones. An index of wedging, which was defined as the posterior length divided by the anterior, showed that in women 48% of the variation in kyphosis can be explained by wedging; and in men 42% of their variation in kyphosis can be explained by wedging.10
Kyphosis has also been related to physical fitness in this study, as well as others. Physical fitness measured either as the Vo2max or muscle strength (via bench press) have each shown inverse significant correlations to the index of kyphosis.7 Muscle strength of the extensors have been studied with positive results. Extensor strength accounted for 11% of the variation in bone density in postmenopausal healthy women.9
Because of the potential relationship to fitness, we reviewed our own available data for exercise habits to search for a relationship to I/K in our sample. These retrospective data, although weak on their own, are useful in suggesting future prospective studies. Women with adequate exercise habits tend to have better posture, less kyphosis.
Previous studies of postmenopausal women showed that age accounts for only 4% more information in the variability of kyphosis10 when the index of wedging has been correlated (via lateral x-rays). Our lack of a continuous age effect are in accord. Survival rate studies revealed that elderly survivors had significantly lower kyphotic index and lower wedging 5 years previously than the group that had not survived. 11
We have used the surveyor's flexicurve in entry physical examinations for a population of well women and have found these measurements easy to carry out. They have provided us with a simple and inexpensive (the flexicurve can be purchased for less than $10.00 and will withstand thousands of measurements) method for the initial evaluation of kyphosis.
ACKNOWLEDGEMENTS
We thank Susan Silverton, MD, PhD at the University of Pennsylvania Metabolic Bone Disease Conference for her many helpful comments and intellectual support. We also thank Celso Ramon Garcia, MD at the University of Pennsylvania, Department of Obstetrics and Gynecology for his very helpful participation and feedback.
REFERENCES
1. Dequeker J., Goris P, Uytterhoeven R: Osteoporis and osteoarthritis (osteoarthrosis). Anthropometric distinction. JAMA 1983;249:1448-1451
2. Ettinger B, Genant H, Cann C: Postmenopausal bone loss is prevented by treatment with low dosage estrogen with calcium. Ann Intern Med 1987;106:30-45
3. Finsen V: Osteoporosis and back pain among the elderly. Acta Med Scand 1988;223:443-449.
4. Levin R: The prevention of osteoporosis. Hosp Pract 1991;May:77-80, 83-86, 91-94
5. Leech J, Dulberg C, Kellie S, Pattee L, Gay J: Relationship of lung function to severity of osteoporosis in women . Am Rev Respir Dis.
6. Bergenuud H, Nilsson B, Uden A, Willner s: Bone mineral content, gender body posture, and build in relation to back pain in middle age. Spine 1989;14:577-79
7. Chow RK, Harrision JE: Relationship of kyphosis to physical fitness and bone mass on postmenopausal women. Am J Phys Med 1987;66:219-227
8. Sinaki M: Postmenopausal spinal osteoporosis: physical therapy and rehabilitation principles. May Clin Proc 1984;57:699-703
9. Sinaki M., McPhee MC, Hodgeson SF, Merret SM, Offord KP: Relationship between bone mineral density of spine and strength of back extensors in healthy postmenopausal women. Mayo Clin Proc 1986;61:116-122.
10. Milne JS, Lauder JJ: The relationship of kyphosis to the shape of vertebral bodies. Ann Hum Biol 1976;3:173-179.
11. Milne JS, Williamson J: A longitudinal study of kyphosis in older people. Age Aging 1983;12:225-233.
12. Cutler WB, Garcia CR: Menopause: A Guide for Women and the Men Who Love Them, ed2. New York, Norton 1992.
13. Garm SM, Solomon MA, Friedl J: Calcium intake and bone quality in the elderly. Ecol Food Nutr 1981;10:131-133.
14. Kanis JA, Passmore R: Calcium supplementation of the diet. Not justified by present eividence. Br J Med 1989;298:137-140.
15. Kanis JA, Pssmore R: Calcium supplementation of the diet. Not justified by present eividence. Br J Med 1989;298:205-208.
16.Thevenon A, Pollez B, Cantegrit F, Tison-Muchery F, Marchandise X, Duquesnoy B: Relationship between kyphosis, scoliosis, and osteoporosis in the elderly population. Spine 1987;744-745.